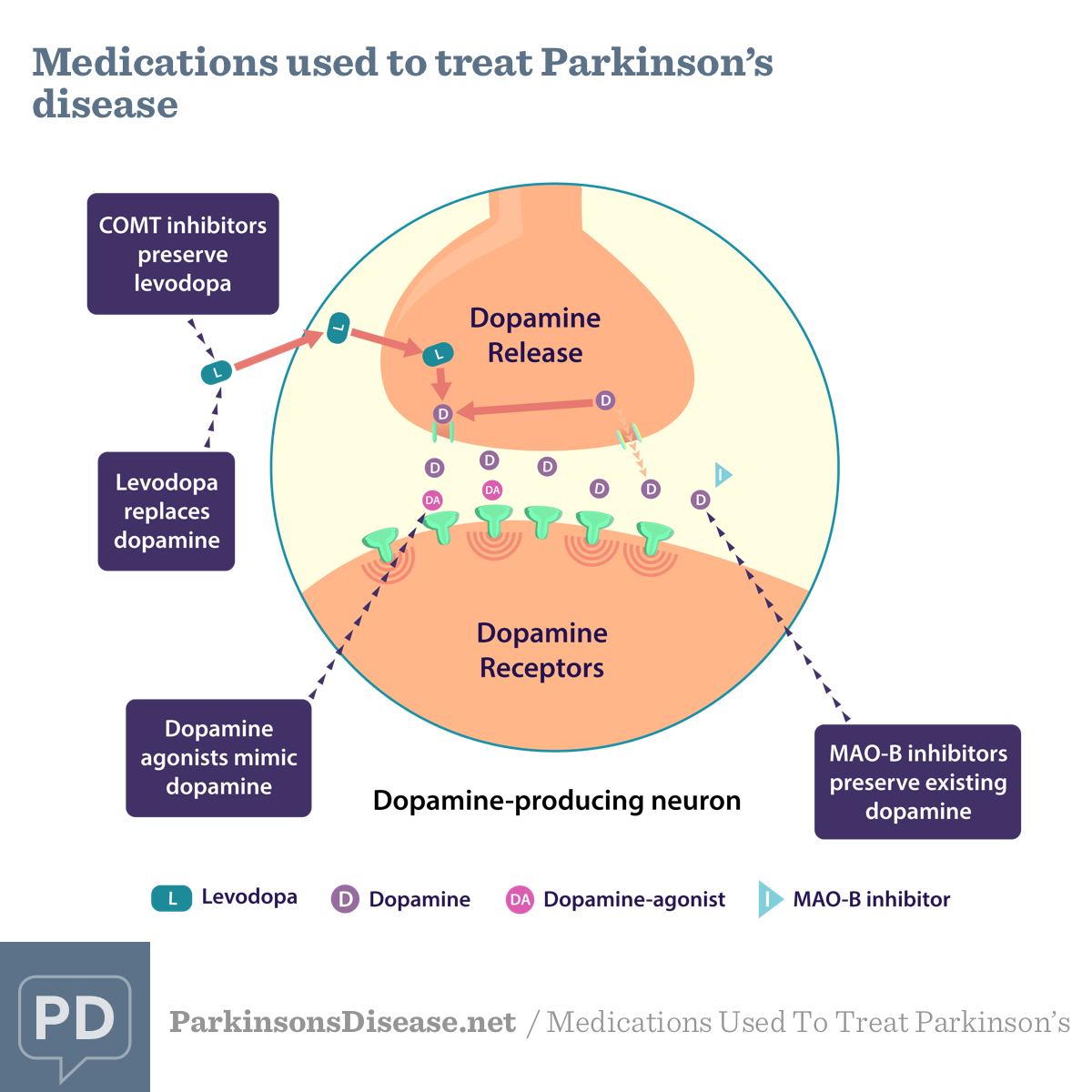
Medications for Parkinson's Disease
Reviewed by: HU Medical Review Board | Last reviewed: April 2025 | Last updated: April 2025
There are several drugs used to help manage the symptoms of Parkinson’s disease (PD). While there is no known cure for PD or any known treatments that can slow the progression of the disease, current research seeks to find ways to stop the progression.1,2
Treatment is highly customized to meet the unique needs of each person since no 2 people with PD are alike. Treatment for PD is focused on:1,2
- Relieving or controlling the symptoms of PD for as long as possible
- Reducing side effects from treatment
- Improving quality of life
Motor symptoms of Parkinson's disease
The motor symptoms of Parkinson's are caused by a lack of the neurotransmitter dopamine in the brain. This causes symptoms like:1,2
- Resting tremor (a tremor or shaking that occurs when a body part is at rest)
- Bradykinesia (gradual loss and slowing down of spontaneous movement)
- Rigidity (stiffness or feeling of tension in the muscles)
- Postural instability (impaired balance)
Drugs for the motor symptoms of Parkinson's disease
There are several different classes of drugs used to treat the motor symptoms of PD, including:1,2
- Dopamine therapy, notably carbidopa-levodopa therapy
- Dopamine receptor agonists
- Anticholinergics
- MAO-B (monoamine oxidase-B) inhibitors
- COMT (catechol-O-methyltransferase) inhibitors
- Amantadine, a mild NMDA receptor antagonist
It is important for people with PD to see a movement disorders specialist who is trained in the use of these drugs for PD. They understand the interactions of these drugs and how some drugs may make symptoms worse.
Carbidopa-levodopa therapy
Dopamine is the chemical messenger that is responsible for smooth, purposeful movement. The main drug treatments used for PD help increase dopamine levels in the brain. By doing so, they help relieve the symptoms of PD. Carbidopa-levodopa provides your body with a molecule that, once in the brain, is converted to dopamine. The combination of levodopa and carbidopa is the most effective treatment available to manage the motor symptoms of PD.1,2
Dopamine receptor agonists
Dopamine receptor agonists mimic dopamine in the brain. This causes neurons in the brain to respond to the dopamine agonists like they would dopamine. This can provide relief from symptoms of PD, especially motor symptoms like tremor, rigidity, impaired balance, and loss of spontaneous movement.3
These drugs are not as effective on the motor symptoms of PD as carbidopa-levodopa therapy. However, they may have fewer side effects.3
Anticholinergics
Anticholinergics block the action of acetylcholine. This is another neurotransmitter involved in messages from the brain to the muscles. Anticholinergics are sometimes used along with other treatments for PD to help manage motor symptoms.4,5
MAO-B inhibitors
MAO is an enzyme found throughout the cells in the body. In the brain, MAO-B plays an important role in the breakdown of neurotransmitters (chemical messengers) like dopamine. MAO-B inhibitors block the action of the enzyme and therefore slow the breakdown of dopamine. Adding a MAO-B inhibitor to levodopa therapy may boost the effect of levodopa by making more of the dopamine it generates available in the brain.3,6
COMT inhibitors
COMT is an enzyme that breaks down neurotransmitters like dopamine. COMT inhibitors block the action of the COMT enzyme and therefore slow the breakdown of dopamine. Adding a COMT inhibitor to levodopa therapy may boost the effect of levodopa by making more of the dopamine it generates available in the brain.7,8
Amantadine
Amantadine is a weak, uncompetitive antagonist of the N-methyl-D-aspartate (NMDA) receptor. While the exact way Amantadine works is not fully understood, scientists think the drug may increase dopamine release and block dopamine reuptake in the brain. This may provide relief from symptoms of PD, especially dyskinesias (involuntary movements) and tremors. Amantadine is also sometimes used to limit side-effects, such as dyskinesias, from dopamine-increasing PD drugs.1,9
Drugs for non-motor symptoms of Parkinson's disease
Other drugs that may be used by people with PD include those that treat specific non-motor symptoms, including:3
- Dementia
- Hallucinations
- Delusions
- Depression
- Orthostatic hypotension (falling blood pressure upon changing positions or standing)